Rural Lives Disrupted by Disease
Rural Lives Disrupted by Disease
Maya Rai, a 38-year-old tea garden worker in Darjeeling, represents the daily struggles faced by many. Her long workdays, combined with household duties, increase exposure to mite-infested environments. When she developed high fever, cough, and fatigue, delayed diagnosis meant she lost several days’ wages before being correctly treated for scrub typhus. Similarly, Ganga Chettri, a homemaker in West Sikkim, faced prolonged hospitalisation, substantial financial costs, and challenges in caring for her young children.
These cases illustrate how delayed diagnosis, lack of awareness, and economic vulnerability exacerbate the human toll of scrub typhus in the Himalayan foothills.
Emergence and Spread of Scrub Typhus
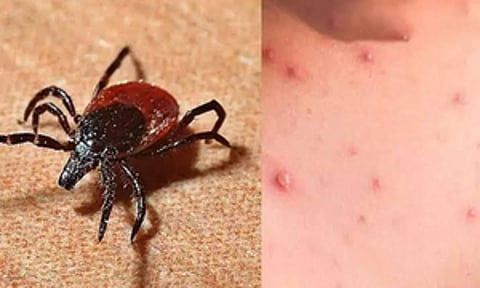
Scrub typhus is caused by the bacterium Orientia tsutsugamushi and transmitted through larval trombiculid mites (chiggers) that feed on small mammals, especially rats. Humans contract the disease when entering mite-infested habitats or areas with dense rodent populations. Environmental factors such as deforestation, land-use changes, urbanization, and waste accumulation increase the likelihood of human exposure.
The Himalayan states of Darjeeling, Sikkim, Himachal Pradesh, Jammu and Kashmir, and Uttarakhand have seen recurring outbreaks since the early 2000s. Darjeeling alone experienced a resurgence in 2005, nearly 45 years after its last documented occurrence. In many regions, scrub typhus accounts for up to 50% of undifferentiated fevers presenting in rural hospitals.
Challenges in Diagnosis and Reporting
Symptoms such as eschar formation, high fever, headaches, muscle pain, and gastrointestinal issues overlap with malaria, dengue, and enteric fever, complicating diagnosis. Rural health centers often lack rapid diagnostic tests, requiring samples to be sent to distant facilities. Patients frequently self-medicate, delaying effective treatment.
Underreporting remains a significant barrier. Private hospitals and rural clinics often struggle to log cases into the Integrated Health Information Portal (IHIP), the government’s central zoonotic disease surveillance system. Limited internet access, understaffed units, and inadequate training hinder timely reporting and outbreak management.
Healthcare Access in Tea Plantations
While the Plantation Labour Act mandates healthcare for tea garden workers, implementation is inconsistent. Provisions mostly cover work-related injuries and general care, leaving gaps in protection against zoonotic diseases like scrub typhus. Reduced permanent staff, declining estate profits, and lack of personal protective equipment further limit access to care.
Integrated Response Needed
Experts advocate for enhanced diagnostic facilities, robust data systems, awareness campaigns, cross-sectoral collaboration, and targeted research to address scrub typhus. An integrated health portal capturing human, animal, and environmental data could strengthen early warning systems and enable timely, evidence-based interventions.
The Himalayan region’s ecological fragility and social marginalization make its populations particularly vulnerable to zoonotic diseases. Focused attention on tea plantation communities, improved healthcare access, and preventive strategies are essential to break the cycle of infection and poverty.